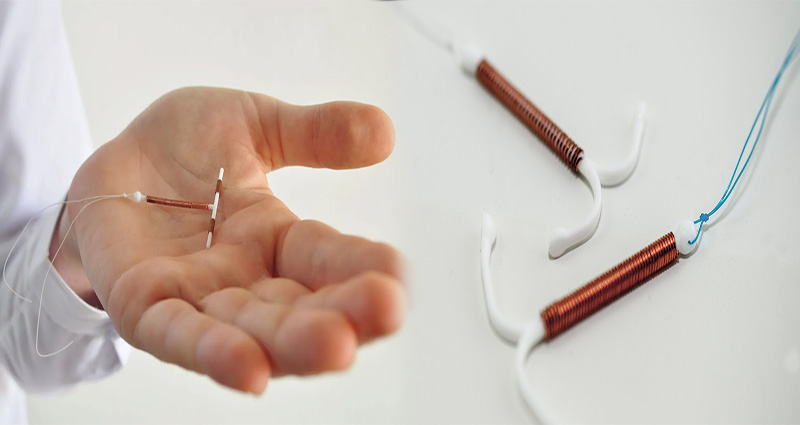
IUDs have been around since the 1960s, but they’re still a relatively new option for American women. An IUD (short for intrauterine device) is a small T-shaped piece of plastic that’s inserted into your uterus by a doctor or nurse practitioner. Once in place, the IUD prevents pregnancy by releasing hormones or copper ions. The hormonal IUD prevents pregnancy by releasing progestin (the hormone found in birth control pills), which makes the cervical mucus thicker and harder for sperm to penetrate. Copper-based IUDs don’t prevent fertilization; instead, they cause a foreign object reaction that causes sperm to die before reaching an egg cell
IUDs are one of the most effective forms of birth control.
IUDs are one of the most effective forms of birth control. They’re over 99% effective, which means that less than 1 out of 100 women will get pregnant each year while using an IUD.
IUDs are also reversible, so if you decide you want to get pregnant or stop using birth control altogether, it’s easy to remove your IUD at any time.
They’re good for five to ten years, depending on the type you get.
Copper IUDs are good for up to 10 years, depending on the type you get. Hormonal IUDs are effective for five years. If you want to keep your IUD indefinitely, ask your doctor about replacing it before its expiration date.
Copper IUDs are T-shaped devices made of soft plastic with copper wires wrapped around the stem; they’re inserted into the uterus by a health care provider and left in place until they need to be removed (usually between 5 and 10 years later). The device prevents sperm from reaching an egg by impeding their movement through the fallopian tubes and fertilizing it once inside an ovary, as well as preventing ovulation from occurring in most women who use them regularly–this means that if a woman does become pregnant while using one of these devices, there’s only a very small chance that it will result in her carrying her pregnancy to term successfully (about 1% per year).
They’re safe for most women and can be used as a form of emergency contraception.
If you’re thinking about getting an IUD, it’s important to know that they’re safe for most women and can be used as a form of emergency contraception. IUDs are not recommended for women who have a history of STDs or pelvic inflammatory disease (PID).
Additionally, some health care providers may discourage the use of copper IUDs by people with heavy periods or endometriosis (a condition in which tissue that normally lines your uterus grows outside it). If you think this might apply to you, talk with your doctor before deciding on one type over another.
There are two types of IUDs — hormonal or copper-based.
There are two types of IUDs — hormonal or copper-based. Hormonal IUDs release small amounts of levonorgestrel, a progestin hormone, into the uterus and fallopian tubes to prevent pregnancy. Copper-based IUDs release copper ions in the uterus and fallopian tubes to prevent pregnancy.
The efficacy rates for both types of devices are very high at more than 99% over five years (meaning less than 1 out of 100 women will become pregnant during that time). However, hormonal IUDs are more effective than copper ones: they have lower failure rates overall as well as lower rates within first year use alone–2% vs 5%, respectively.*
Because both types work differently in terms of how they prevent fertilization from occurring, you may experience different side effects depending on which one you choose!
You should be screened for STDs before getting an IUD.
You should be screened for STDs before getting an IUD. While the risk of STDs is low, it’s important to be screened if you are at risk or have a history of STDs. If you’re found to have an STD, your doctor may recommend treatment or abstinence from sex until your infection is cleared up.
If you do not have sex with men, but still want protection against pregnancy and/or STDs, consider asking about getting the ParaGard IUD instead of Mirena (which can also be used as an emergency contraceptive).
An IUD might be right for you if you want long-term birth control without hormones.
- IUDs prevent pregnancy in three ways: they prevent sperm from entering the uterus, they prevent eggs from being released and they make it difficult for a fertilized egg to implant in the uterus.
- An IUD is a good option if you want long-term birth control that doesn’t contain hormones. Hormonal birth control methods like the pill and patch have been linked with certain health risks (like blood clots), but there’s no evidence that suggests an increased risk of cancer or heart disease for people who use nonhormonal methods like an IUD or a copper IUD (which releases no hormones).
- If you’re looking for something more discreet than condoms or pills that are easy to use on your own time–and don’t mind having something inserted into your body–an IUD may be right for you!
IUDs are an excellent option for women who want long-term birth control without hormones. If you’re considering getting an IUD, make sure to talk with your doctor about the pros and cons of this type of birth control. They can be used as emergency contraception up to five days after unprotected sex, so if that sounds like something you might need (or just want), then it’s worth looking into!